Pulmonary Thromboembolism as a Complication of Systemic Lupus Erythematous and Antiphospholipid Syndrome
Mohamed Teleb, Komola Azimova, Miraie Wardi, Mateo Porres-Aguilar, Debabrata Mukherjee
Med Sci Case Rep 2015; 2:33-37
DOI: 10.12659/MSCR.894649
Available online: 2015-06-27
Published: 2015-06-27
BACKGROUND:
Antiphospholipid syndrome (APS) is an autoimmune disease characterized by tiphospholipid antibodies (APA) in the presence of arterial or venous thrombosis. These autoantibodies are often detected in systemic lupus erythematous (SLE), and thus APS and SLE may coexist. Acute pulmonary thromboembolism (PTE) is a common presentation of APS, occurring in approximately 40% of patients. However, chronic PTE occurs only in a small percentage of patients with APA. It can lead to progressive pulmonary hypertension and permanent pulmonary vascular changes. Here, we present the case of a 47-year-old woman who presented with chronic PTE as a complication of SLE and APS.
CASE REPORT:
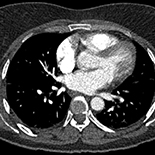
We present the case of a 47-year-old woman with no significant past medical history who presented to the emergency room with chest pain and shortness of breath. Further evaluation and imaging studies revealed chronic PTE. Work-up of the main cause led to the diagnosis of APS and SLE. She was started on a full dose of enoxaparin and bridging with Coumadin. She was also prescribed hydroxychloroquine and prednisone with rheumatology follow-up. She was discharged in a stable condition.
CONCLUSIONS:
APS and SLE are associated with chronic PTE. It is an important sequela but a rare entity of the disease that can lead to chronic pulmonary hypertension. Early detection is important to prevent further complications. Treatment consists of life-long anticoagulation therapy or other options such as lung transplantation if medical treatment failed.
Keywords: Antibodies, Antiphospholipid, Antiphospholipid Syndrome, Lupus Erythematosus, Systemic





